The SMART way to achieve effective decontamination and sterilisation of dental handpieces in daily practice
The effective decontamination of dental handpieces presents a challenge, notably the cleaning of hidden internal surfaces and hollow channels (lumens). As sophisticated instruments with precision-engineered moving parts, they must be decontaminated and maintained with meticulous care, which includes putting them through a cleaning, lubrication and sterilisation process after every use.
Failure to reprocess handpieces correctly not only compromises patient and staff safety but also restricts performance and reduces their potential lifespan. Handpieces are routinely contaminated with blood, saliva and biological residues, making them a potential transmission risk of a host of bacterial and viral infections including Covid-19 and blood-borne diseases including Hepatitis B, C and HIV. The decontamination team, therefore, require robust processes and reliable equipment that will help them not only to meet but exceed industry-wide decontamination standards.
Start the SMART way
The NSK SMART3 handpiece decontamination protocol offers a safer, more measured and cost-effective process, one that is reproducible and time-saving. By adopting a SMART3 approach: 1. Cleaning 2. Lubrication 3. Sterilisation – it is possible to ensure effective decontamination and sterilisation of all instruments, especially handpieces, as well as maintaining their peak performance and lifespan.
1. The cleaning process
![]() The aim of the cleaning process is to ensure surfaces are free of debris and matter so that sterilisation can be effective, as any remaining contaminants will act as a barrier to steam penetration. It is important to remember that if something is not clean it cannot be sterilised, therefore all contaminants on the external surfaces of handpieces and instruments should be removed immediately after use.
The aim of the cleaning process is to ensure surfaces are free of debris and matter so that sterilisation can be effective, as any remaining contaminants will act as a barrier to steam penetration. It is important to remember that if something is not clean it cannot be sterilised, therefore all contaminants on the external surfaces of handpieces and instruments should be removed immediately after use.
External surface cleaning can be performed manually, under cold running water using a soft to medium, non-metallic brush. Surfaces should then be disinfected with a good quality disinfectant wipe. Any residue should be rinsed off under cold running water in a separate cleaning sink, then dried with a clean tissue or paper wipe. After a careful, visual inspection, they are ready to be cleaned internally.
Effectively cleaning both the external and most importantly, the internal surfaces and lumens of a handpiece are best achieved using a dedicated handpiece cleaning and lubrication unit such as the NSK iCare. These automated systems are designed to quickly and effectively remove dirt and debris from the internal workings, using tried and tested solutions to deliver the precise amount of lubrication to all parts of the mechanism, including internal lumens, in preparation for subsequent sterilisation. This should always be carried out following the handpiece manufacturer’s guidelines.
2. The lubrication process
![]() As with internal cleaning, a manual process is not always the most effective way to lubricate a handpiece, especially as it relies heavily on the diligence of the operator to ensure the proper steps are taken.
As with internal cleaning, a manual process is not always the most effective way to lubricate a handpiece, especially as it relies heavily on the diligence of the operator to ensure the proper steps are taken.
An automated cleaning and lubrication unit dispenses the precise amount of lubricant every time. With the connection to a source of compressed air, any residual contaminants, solutions, and lubricants that could compromise sterilisation are automatically purged from inside the handpiece at each stage of the cycle in just seconds. This measured, effective and reproducible process means handpieces are turned around faster, inventories are better managed and the overall process is less prone to human error.
3. The sterilisation process
![]() Steam sterilisation is the essential next step after cleaning and lubrication for the reprocessing of handpieces that have become contaminated with saliva, blood or other biological fluids.
Steam sterilisation is the essential next step after cleaning and lubrication for the reprocessing of handpieces that have become contaminated with saliva, blood or other biological fluids.
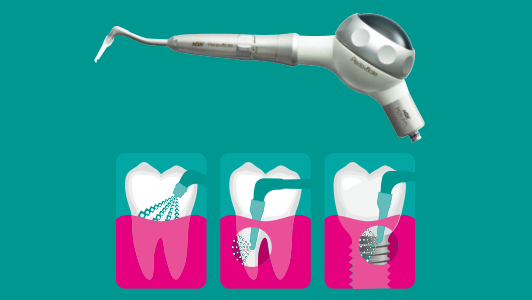
Sterilisation aims to break the chain of potential cross-contamination between patients by killing microorganisms, including any viruses, bacteria and fungal spores that may otherwise cause infection or disease. The recommended method of sterilisation of hollow handpieces such as turbines and contra-angles, is by using the correct, validated autoclave cycle that delivers saturated steam, under pressure at the highest temperature compatible with the load, typically 134-137° for at least a three-minute holding time.
Sterilisation requires direct contact between saturated steam and every surface of the instrument – inside and out. However, because of the complexity of hollow instruments including handpieces and pouched loads, effective steam penetration and sterility will be compromised by the presence of air within the instrument or sterile packaging. Therefore it is imperative all air is actively removed from the chamber and load when processing anything other than solid, unwrapped instruments (ref: HTM 01-05: 4.5).
www.the-probe.co.uk Active air removal can only be achieved in an autoclave that creates a state of vacuum before sterilisation using a vacuum pump to forcibly remove the air as opposed to a non-vacuum autoclave which relies on gravity or downward displacement by steam to passively remove the air from the chamber and load.
Autoclave cycle types
There are three types of autoclave cycles:
- Type N autoclave cycles: these rely on displacement by steam to achieve air removal. Research has shown (Winter et al.) they do not reliably sterilise hollow or pouched instruments, making them only suitable for unwrapped or solid items.
- Type S autoclave cycles: These are defined by the manufacturer to take specific loads through a sterilisation process including handpieces and pouched instruments where stated. Type S autoclaves use vacuum-assisted, active air removal and should only be used following the manufacturer’s instructions.
- Type B autoclave cycles: These meet a defined standard i. e. EN 13060 that specifies the performance requirements and test methods for small steam sterilisers and sterilisation cycles. Type B autoclaves almost always employ vacuum pumps to effect active air removal and steam penetration. This makes them suitable to process a wide variety of load types including hollow, air retentive and packaged loads including hollow instruments in sealed packaging.
A handpiece that has been correctly cleaned and lubricated and excess solution and lubricant is purged from the instrument before sterilisation (as when using an automated handpiece cleaning and maintenance unit), as long as all the air has been removed, steam will be able to penetrate the instrument and take it through a sterilisation process. Therefore, the appropriate S or B-type vacuum autoclave cycle must always be used to sterilise handpieces.
Additional benefits
Sterilisation performance can be further improved by using a vacuum autoclave that incorporates a copper chamber, such as the NSK iMax S S type autoclave or the advanced NSK iClave plus B type vacuum autoclave. Copper, being more thermally efficient than stainless steel offers additional user benefits:
- Improved performance both in terms of cycle speed and drying
- Improvements to the efficiency of the drying phase helps eliminate many handpiece care and maintenance issues, including corrosion and discolouration
- Improved levels of reliability and serviceability can lead to the ongoing reduction in instrument and autoclave maintenance costs
The SMART solution
As the UK’s market leader in handpiece and decontamination technology, NSK is committed to improving the standards of handpiece decontamination as well as providing support to our customers in optimising their handpiece decontamination process.
The NSK SMART3 handpiece decontamination protocol makes the three crucial decontamination steps of cleaning, lubrication and sterilisation Safer, Measured, Affordable, Reproducible and Time-saving.
Reducing the risk of manual error and inconsistencies by the use of equipment specifically designed for each part of the decontamination process ensures not only that best practice can be achieved but it can be reproduced every single time.

About the author
Mark Beckwith is NSK’s
Decontamination Consultant.